In light of the current measles epidemics spreading in Europe, I wanted to visit some of the main concerns with the disease, and the reasons we very fervently want to put a stop to its spread. Seven reasons to make sure you protect yourself and your children from measles:

- Diarrhea, ear infection, and hearing loss. Common measles complications.
- Pneumonia. Occurs in about 1 in 20 children, most common cause of death from measles in young children.
- Encephalitis (swelling of the brain). About 1 out of every 1,000. Can lead to convulsions, deafness, or intellectual disability.
- Death. Estimated between 1-10 in every 5,000 cases of measles, or up to 1 in 10 where adequate nutrition and health care are lacking.
- Immune amnesia. Measles is associated with two years of increased susceptibility to, and mortality from other infectious disease. Studies suggest measles causes ‘immune amnesia’, wiping out previously developed immune memories.
- Delayed fatal inflammation of the brain (SSPE). Occurs 2-4 years after measles. May be much more common than thought, 1-2 per 10,000 – and a preliminary report warns of rates even higher, 1 in 600 for children under one year and, 1 in 1,400 in up to five-year-olds.
- Epidemics. Measles is one of the most contagious of all infectious diseases. It is infectious before symptoms appear and remains in the air two hours after infectious person has left. The sick and the very young and old, will always be easy victims of measles.
Measles basics
The World Health Organisation 2015 statistics show a total of 195’762 reported cases of measles, although the actual number is bound to be much higher, and they estimate there to have been 134’200 deaths from measles worldwide, making measles the fifth most common cause of mortality among children.
Measles is one of the most contagious of all infectious diseases, infecting circa 9 out of 10 of every susceptible person who has close contact to a measles patient. The CDC tells us that:
The virus is transmitted by direct contact with infectious droplets or by airborne spread when an infected person breathes, coughs, or sneezes. Measles virus can remain infectious in the air for up to two hours after an infected person leaves an area.
CDC estimates that 3-4 million people in the US were infected with measles yearly before vaccine introduction – almost all children. Most of the cases were not reported, but there were close to 500,000 reported ones annually before 1963. These cases resulted in:
- 48,000 hospitalizations – 1 in 10
- 4,000 cases with encephalitis (brain swelling) – almost 1 in 100
- 450 to 500 deaths – 1 in 1,000
England and Wales health officials have similar data, with about 2 mortalities per 1,000 measles cases before the 1950s. The death rates in England and Wales drop below one per thousand in more modern times, and current estimates of the UK NHS is a mortality rate of 1 per 5,000, whereas a 55,000-case outbreak in the US in 1989-1991 had a mortality rate of bit more than 2 per 1,000 (123 deaths all in all).
Based on what we know about the reported half a million cases annually in the US, and the estimate of the total number of measles cases per year of 3-4 million, the real death rate in the US could have been 3000-4000 per year. The cases that were not reported may also have included more people living in poorer situations, and their measles death rates might even have been higher, considering the WHO estimates:
In populations with high levels of malnutrition and a lack of adequate health care, up to 10% of measles cases result in death.
While vaccine fears are bringing back measles epidemics in the west, however, measles vaccination programs are having tremendous effect at curbing the disease in the developing world:
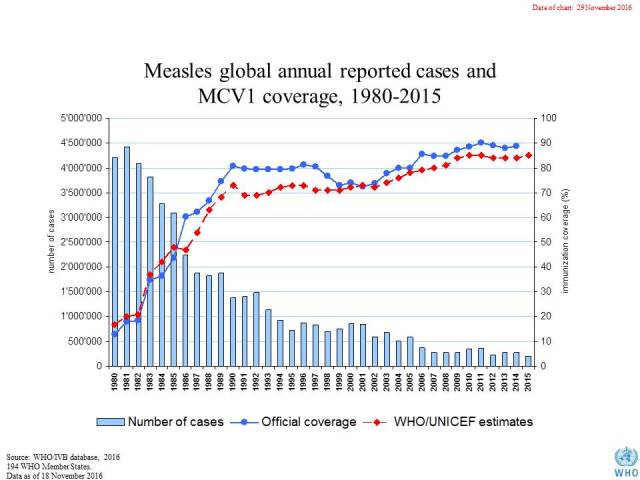
Luckily global vaccination programs have had a drastic effect on measles worlwide. Source: the WHO.
Immune amnesia – two year reset of the immune system
A 2015 study tracked real world incidence of measles and other infectious disease, and found a profound effect in overall ability to fight disease following a measles infection:
Immunosuppression after measles is known to predispose people to opportunistic infections for a period of several weeks to months. Using population-level data, we show that measles has a more prolonged effect on host resistance, extending over 2 to 3 years.
This seems to be the promising missing piece in a long-time puzzle of the general dip in disease statistics following wide-spread vaccination programs: after measles vaccinations, all cause mortalities dropped as well. NPR reports on it at Scientists crack a 50 year old mystery about the measles vaccine:
Back in the 1960s, the U.S. started vaccinating kids for measles. As expected, children stopped getting measles.
But something else happened.
Childhood deaths from all infectious diseases plummeted. Even deaths from diseases like pneumonia and diarrhea were cut by half. […] “So it’s really been a mystery — why do children stop dying at such high rates from all these different infections following introduction of the measles vaccine,” he says. […]
“We found measles predisposes children to all other infectious diseases for up to a few years,” Mina says.
The concept of measles ‘immune amnesia’, or measles immune suppression, is not new, however, and has been studied for decades, although its effects have earlier been thought to last weeks or months, rather than years. Even so, the prolonged immune suppression has long been considered to be responsible for measles’ most debilitating effects. From a 2004 review:
Deaths from measles are due largely to an increased susceptibility to secondary bacterial and viral infections, attributed to a prolonged state of immune suppression. Several abnormalities of the immune system have been described, including changes in lymphocyte number and function, shifts in cytokine responses, immunomodulatory effects of interleukin-10, down regulation of interleukin-12, impaired antigen presentation, and altered interferon alpha/beta signaling pathways.
The most recent review, from 2013, looks more into the mechanisms, and notes that: “The morbidity and mortality of MV is associated with severe immune suppression.”
Measles’ immunosuppressant properties have also been studied in macaque monkeys: Measles Immune Suppression: Lessons from the Macaque Model:
The rapid oligoclonal expansion of MV-specific lymphocytes and bystander cells masks this depletion, explaining the short duration of measles lymphopenia yet long duration of immune suppression.
And as if this bummer of a immune-reset from measles would not be bad enough, recent research has also found the risk of a grave side effect, SSPE to be much larger than previously considered.
Fatal brain inflammation, SSPE
A mild and uncomplicated case of measles can lead to a dormant measles infection of the nervous system, which reactivates years later, causing subacute sclerosing panencephalitis or SSPE. It is a progressive neurological disorder that leads to death generally within a year or two of diagnosis. More about that in Science Based Medicine: SSPE: A Deadly and Not-That-Rare Complication of Measles. The SSPE rate, previously estimated at a few cases per 100,000, was found to be 1-2 in 10,000 in a study of a US measles outbreak in 1989-1991. An recent piece in the Scientific American reports of a yet-unpublished study of the 1998-2015 data in California, where rates were found to be even higher. Deadly Measles Complication More Common Than Doctors Thought:
…new analysis suggests that kids who get the measles before age 5 have a one in 1,387 chance of developing SSPE, and kids who get the measles before age 1 have a one in 609 chance. […]
In the study, the researchers looked at all of the cases of SSPE in California that occurred between 1998 and 2015, identifying 17 cases. The children were diagnosed with SSPE, on average, at age 12, the researchers found.
Any of the above measles complications is an unnecessary and a cruel burden to put on a child (or a parent) when there is such an easy and safe alternative that provides great protection against the disease.
Measles vaccination is a safe
Australian Immunisation Handbook provides a side-by-side look at the risks from the diseases vs the vaccines that protect from them. For measles, they report (using the old, more conservative estimate of SSPE rates):
About 1 in 15 children with measles develops pneumonia and 1 in 1000 develops encephalitis (brain inflammation). For every 10 children who develop measles encephalitis, 1 dies and many have permanent brain damage. About 1 in 100 000 develops SSPE (brain degeneration), which is always fatal.
The measles vaccine is painstakingly safe in comparison to the serious realities of measles itself:
About 1 in 10 has local swelling, redness or pain at the injection site, or fever. About 1 in 20 develops a rash, which is noninfectious. Low platelet count (causing bruising or bleeding) occurs after the 1st dose of MMR vaccine at a rate of about 1 in 20 000 to 30 000. Serious adverse events are very rare.
For easy infographic comparisons of vaccine vs disease risks, for measles and others, please see the collection made by The Mad Virologist.

As confirmed by a recent study of 25 million vaccines administered between 2009 and 2011, severe reactions to vaccines are indeed very rare. Out of these 25 million instances, vaccines caused 33 cases of anaphylaxis, but none were fatal. No children under 4 were affected. Most cases (85 %) had a history of allergies, asthma or anaphylaxis. Thus they confirmed once more the known rate of severe allergic reactions to vaccines, which is approximately 1 per million.
Measles vaccine has at one point been falsely connected to autism on the basis of one fraudulent study whose author, Andrew Wakefield, had significant predetermined monetary motives, and who lost his licence for misconduct.
Autism in children is often not confirmed or properly detected until after the first year of life, so parents may easily grab hold of different things that happen around then to find something to explain the diagnosis, even if the actual changes leading to autism development have occurred before birth – you can read much more about that in my piece The Great Myth of Vaccines and Autism.
Bottom line is, that there has never been any actual evidence of a connection. Sadly after this falsified study, parents fears have been dishonestly flamed, making many anxious about vaccinating. To reassure them, during the last decade and a half more than 14 million children have been included in a wide array of autism studies, and their conclusions are clear: no connection between vaccination and the development of autism can be found.

For more, see The Great Myth of Vaccines and Autism
Not only is the vaccine safe, but it also does a great job at what it’s supposed to do: protecting from measles and all of its complications.
Measles vaccination is effective
Measles was somewhat constant in prevalence in the US through 1910-1940, but during this time, better nutrition and hospital care began to help alleviate its worst effects, lowering the number of fatalities. Unfortunately complications such as encephalitis, deafness, and pneumonia, etc, still occurred often – all in all resulting in about 1 death per 1,000 – and before the vaccine, nothing had been able to stop the infection of hundreds of thousands to millions of people (mostly children) every year in the US alone. After the vaccine was introduced, however, measles cases plummeted.
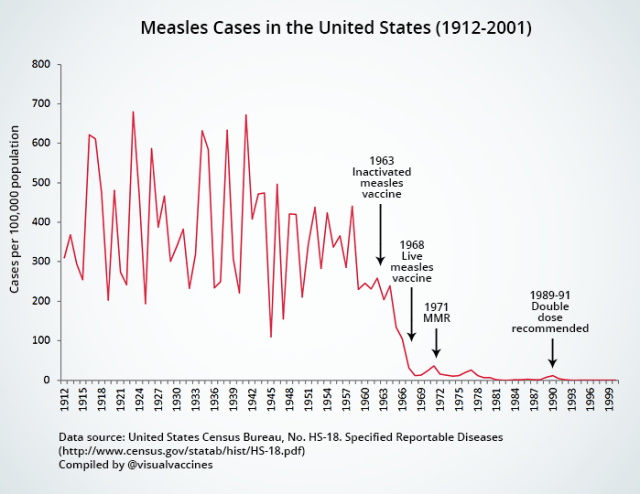
Graph by Visual Vaccines – visit to view sources and many more graphs.
I’ll also include the graph of measles vaccine introduction in England and Wales. This graph I find particularly interesting because it shows an effect similar to one known in research as the “dose-response” relationship – a very robust method of determining causality.
Here we can follow the effect of gradually increasing vaccination rates (the dotted line), and see that as more people that got the vaccine, the fewer became the cases of measles. The graph also shows the dip in the vaccination rates, as they venture below 90% soon after Mr Wakefield began fuelling the fears of the anti-vaccine campaigners around the beginning of the century. The epidemics in the UK have so far only reached little over a thousand cases per season, and are thus luckily but a slight bump at the end of the red curve:
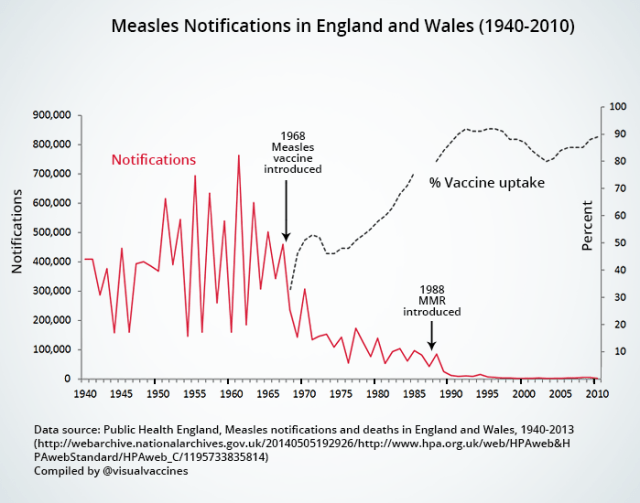
Graph by Visual Vaccines
Those most vulnerable will always rely on herd immunity
Measles vaccine is about 97 % effective. This means that there are on average three unlucky individuals out of a hundred who won’t develop an adequate immune memory to measles, and will continue to be susceptible to the disease.
It is important to note that there will always be additional groups of people who will have to rely on herd immunity rather than individual immunity to stop disease, such as:
- People without a fully-working immune system, like those without a working spleen
- People on chemotherapy treatment whose immune system is weakened
- People with HIV
- Newborn babies who are too young to be vaccinated
- Elderly people
- Many of those who are very ill in hospital
The percentage of immune people in the community necessary for a measles infection to be extinguished is roughly 95%. So when more than 5% of people are skipping their shot, they are not only affecting their own child’s disease protection, but are bringing back the disease epidemics which may again reach all the vulnerable people in the community.
The vaccination rate that is critical for stopping the spread of disease depends on how infectious the disease is – measles is highly contagious, a sick person infecting on average 11-18 people in turn, and this is why such a high vaccination rate is necessary to keep its epidemics entirely at bay. You can read more about it over at my piece on The Simple Math of Herd Immunity, but for a quick visual presentation of the herd immunity effect, watch this great animation of measles spreading in populations with different vaccination rates over, at The Guardian: Watch how the measles outbreak spreads when kids get vaccinated – and when they don’t.
Recent epidemics demonstrate effects of the anti-vaccine movement
In the past decades, with the British Andrew Wakefield fuelling anti-vaccine propaganda, Measles, Mumps and Rubella vaccine-uptake has been lagging well behind the required 95 % coverage – around 70-80% in several countries – although hopefully, many are on the way up again.
Meanwhile, the effects are here today: measles is on the march again in Europe. In the past year in Romania, more than 2,000 cases have lead to 17 deaths. Italy, France, and Germany have reported tens or hundreds of cases in the past few months, and Switzerland just had its first measles death since 2009. The number of cases in Europe for the month of January 2017, as well as the vaccination rates for 2014-2015 tracked by the WHO, can be viewed below.
UPDATE: As of May Italy has more than 2000 cases in 2017. Newest stats for the Romanian outbreak, from January 2016 to 12 May 2017: total 5 728 cases including 25 deaths. More here.
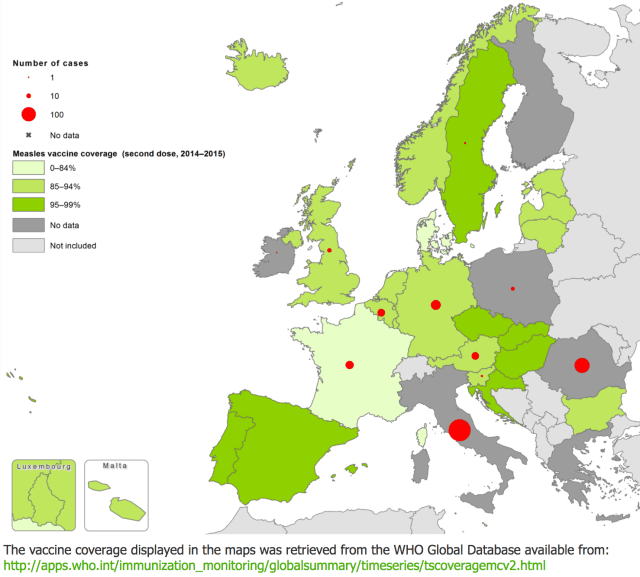
Note, some countries lack vaccination data in the map because report only on coverage of one dose of measles vaccine. In the Nordic countries, where vaccine rates have traditionally remained high (and where I am from), measles cases of the last year can be counted with one hand, but Switzerland (where I am a resident) has been lagging behind, with 71 % vaccine uptake as recently as in 2010, reports 52 cases of measles in the first three months of 2017 alone.
Some have suggested that measles epidemics might be the result of a flux of immigrants and refugees, rather than national vaccine-refusal, but most refugees arriving in Europe today come from countries with high vaccination rates. The WHO has traced the current epidemic to Romania’s anti-vaccine pockets, as Layla Katiree lays out in her piece Blame Disease Outbreaks On Vaccine Avoidance, Not Refugees:
Romania’s measles outbreak began in February 2016, and measles cases in Europe have been linked to individuals who travelled to Romania (see here and here).” […]
Despite the recommendation from WHO, Romania’s vaccination coverage for the first dose of the MMR vaccine was estimated to be 88% in 2015, with a wide range in coverage across the nation. The World Health Organization states that these pockets of suboptimal immunization rate around the country are due to “certain cultural traditions, religious beliefs, fear of adverse effects of the vaccine or lack of confidence in public authorities”. The recent outbreak finds the majority of its cases in regions of Romania “where immunization coverage is especially low”.
For more data on measles cases vs immunization rates, and surveys of anti-vaccine views, check out this recent article from Euronews, or browse the reported vaccination rates for different vaccines in this vaccine coverage catalogue from the WHO – choose MCV1 or MCV2 for the two measles vaccines, and you can see the trends in vaccination per year per country.
The European statistics on the surge in measles from a few years ago, in 2012-2013, demonstrates the impact of anti-vaccination: 83 % of cases were in entirely unvaccinated, and only o.4 % of the cases in fully vaccinated people.
Vaccination status was known for 95% of the 10 675 cases reported with known age. Of these 10 129 cases, 83% (8 910 cases) were unvaccinated, 8% (826) had received one dose of measles vaccine, 0.4% (42) had received two or more doses, and 3% (351) had received an unknown number of doses.
Three measles-related deaths were reported during the period November 2012 to October 2013, and eight cases were complicated by acute measles encephalitis.
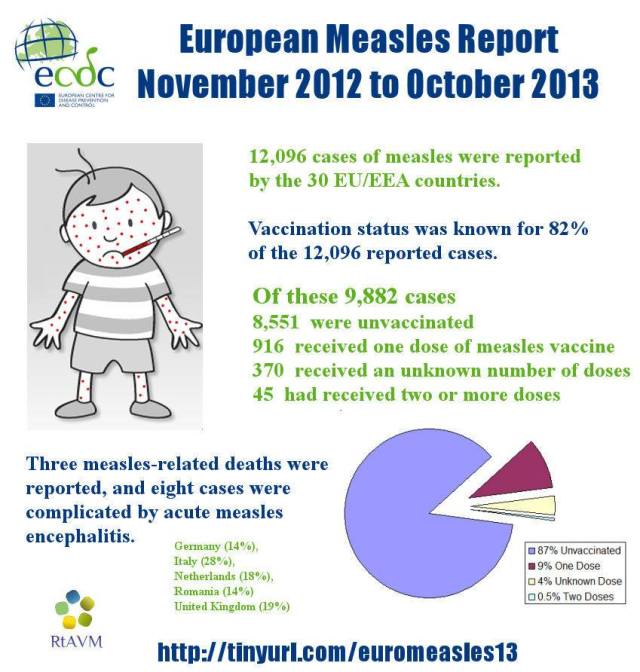
Thanks to Refutations to Anti-Vaccine Memes for the graphic on the WHO data
It is a sad possibility that this may be the only way some parents will be convinced of the benefits of vaccinations: by coming face to face with the reality of returning epidemics, resulting in death and disability for children, who will be the needless victims of vaccine-fears.

If you’d like to read more, see my articles and infographics under: Vaccines and Health. If you would like to discuss the topic below, you are very welcome, but please take note of my Commenting policy.
In a nutshell:
- Be respectful.
- Back up your claims with evidence.

Pingback: A Tribute to My Grandmother, A Survivor of War, and a Pioneer Science Communicator 1950-1980 | Thoughtscapism